|
One of the
best Australian sites I have seen on the net is
The Paralysis Tick of
Australia. This site has extensive information. Well and truly worth a visit. Be prepared to spend some time here!
The main Tick species in Australia include:
The Indigenous Tick - found in Western Australia, Tasmania, the south-east coastal region of New South Wales and central Victoria. It may cause paralysis.

Paralysis Tick - found from northern Queensland to Bairnsdale in Victoria along the coastal regions. Causes paralysis.
Cattle Tick - found in Queensland, north-eastern New South Wales, Northern Territory and Western Australia. This tick is rare on dogs and carries parasites found in cattle blood.
Bush Tick - also known as a scrub tick and New Zealand cattle tick. It is found in the southeast coastal area of Queensland, along the New South Wales coast line and through north eastern Victoria along the Murray River.
Brown Dog Tick - (Click here
for more information) found mainly in inland areas of Queensland, Western Australia, New South Wales and Victoria. Most prevalent in the northern parts of Australia. Carries a wide range of infectious diseases including Babesia Canis which can occur in a symptom less carrier state or in disease form ranging in severity from mild to severe and occasionally causing death.
Other ticks found in Australia include the Cat Tick, Possum Tick, Opossum Tick and the Wallaby Tick.
 The AUSTRALIAN PARALYSIS TICK (Ixodes
holocyus) is distributed in south eastern coastal temperate regions. It secretes a neurotoxin in its saliva that causes a progressive, and occasionally fatal, paralysis. Sometimes a severe hypersensitivity reaction may occur. Often the tick goes unnoticed until weakness or ataxia develop, and then is found during an ensuing search (don't forget to look behind ears etc!). Occasionally localised paralysis of facial muscles occur, but more commonly there is progressive ascending flaccid paralysis affecting the lower limbs first. Other grass ticks can be a real nuisance at times, causing really itchy bites. The AUSTRALIAN PARALYSIS TICK (Ixodes
holocyus) is distributed in south eastern coastal temperate regions. It secretes a neurotoxin in its saliva that causes a progressive, and occasionally fatal, paralysis. Sometimes a severe hypersensitivity reaction may occur. Often the tick goes unnoticed until weakness or ataxia develop, and then is found during an ensuing search (don't forget to look behind ears etc!). Occasionally localised paralysis of facial muscles occur, but more commonly there is progressive ascending flaccid paralysis affecting the lower limbs first. Other grass ticks can be a real nuisance at times, causing really itchy bites.
Prevention is better than cure. If you know you are going into tick areas, wear long, light-coloured trousers and tuck them inside tight socks. If you look out for ticks crawling up the outside of your trouser legs you can brush them off before they get inside.
|
|
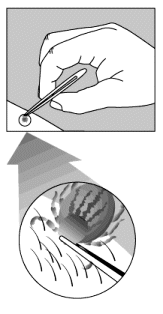 If a tick is removed within 24 hours, the chances of it transmitting Lyme disease or other infections are much less. The illustrations (right) show how to remove a tick properly. Use fine-point tweezers to grasp the tick as close to the skin as possible. Pull gently. Avoid squeezing the body of the tick. Clean the site of the bite, your hands and the tweezers with disinfectant. You may want to wear protective gloves. If a tick is removed within 24 hours, the chances of it transmitting Lyme disease or other infections are much less. The illustrations (right) show how to remove a tick properly. Use fine-point tweezers to grasp the tick as close to the skin as possible. Pull gently. Avoid squeezing the body of the tick. Clean the site of the bite, your hands and the tweezers with disinfectant. You may want to wear protective gloves.
Removal of the tick can be achieved in many different ways. Never grip the the sac and pull! This may squeeze more venom in, or break the it off and leave the head and 'torso' firmly stuck, which is likely to get infected. These days most people recommend gripping the tick as near to the head as possible with a very pointy pair of tweezers or forceps. Ordinary eyebrow tweezers are not much good because the points are too wide. You can make them more effective by filing the tips away to a sharp point. For larger ticks I personally like making a 'loop' or 'noose' from a piece of cotton thread with a single throw knot (half of a reef knot). This is placed at the base of the body, then slowly and gently closed until it won't slip over the body. Then
gently pull on the free ends of thread with a 'to-and-fro' rocking motion until the whole tick comes out. Nothing entertains children more than seeing the little wriggling legs of the removed tick - except the satisfaction of finally squishing the beast!
Try to avoid leaving the head in, as it will become infected. Remember, DO NOT try to pull the tick out by gripping the end part of the body! This almost always breaks off and fails to remove the head and legs.
Ticks usually have a firm hold on you once they have dug in. Additionally, there can be quite a lot of swelling around them. This can make them difficult to remove, and so many people have sought means to induce them to 'let go' by themselves, or at least to cause them to 'relax their grip'.
Whatever you do, make sure you kill them afterwards.
For extra protection after removing the tick, dab the area with a topical antiseptic like Betadine Solution or an antibiotic ointment.
If the patient has developed severe symptoms, apply the pressure and immobilisation technique until they can receive antitoxin.
You also may want to place the tick in a small container, like a pill container, and
take it to your vet for identification. Never use a burned match, petroleum jelly, or nail polish to try to remove ticks. These methods are ineffective. |
|
BABESIOSIS
Babesiosis is caused by a protozoan (single-celled) parasite known as a piroplasmid, namely Babesia canis. During its life cycle, this parasite must pass through a vector host before transmitting the disease from one dog to another. The vector is the female tick.
Parasitic development in dogs has several stages corresponding to changes in the parasite. At first, the parasite is a very simple, circular organism known as a trophozoite. It enters the red blood cells and feeds on their
haemoglobin, which it digests. The trophozoite undergoes asexual reproduction (simple cell division). The nucleus of the cell divides first, then the membrane and cytoplasm (the liquid contained within the membrane). The division results in two droplet-shaped daughter cells, or merozoites, which are still inside the red blood cell.
There may be more than two cells inside one red blood cell. Usually, the red blood cell is destroyed after division and the merozoites are released into the bloodstream. Each merozoite quickly attaches to another red blood cell, enters it, and forms a trophozoite. Some piroplasmids, called gamonts, stop dividing in the red blood cells.
The tick, an intermediate host, takes a meal on an infested dog. The red blood cells it ingests are destroyed in its intestine, as are the trophozoites and merozoites. Only the gamonts remain, which become gametes in the intestinal wall. Two gametes fuse, forming an egg, or zygote. The zygote produces a motile form that leaves the tick's intestine to enter its egg cells, where it multiplies and gives rise to motile spores. If a female tick in the next generation, i.e., one arising from an egg containing motile spores, bites a dog, the motile spores move into her salivary glands. Each motile spore becomes very large, and is then called a sporont. Inside the sporont, thousands of sporozoites form and infest the dog. Each sporozoite enters a red blood cell and becomes a trophozoite to complete the cycle.
Babesiosis is especially frequent in hot and temperate climates, in areas where ticks are abundant. It is more widespread during seasons in which ticks are active, and with certain lifestyles, as in hunting dogs. Highly-selected breeds such as Cocker Spaniels, spaniels, Yorkshire Terriers, and Dobermans are more susceptible than others. Puppies are more vulnerable than adults.
The incubation period, which corresponds to the period during which the parasites are multiplying in the dog's body, can last from two days to about two weeks. During this stage, no piroplasmids are present in the blood. After this stage, the parasites appear in the blood and symptoms appear almost simultaneously. In the acute form of this disease, the dog has a very high fever and is exhausted. The fever lasts an average of six to ten days. At the same time, anemia (pallor of the mucosa) is present due to the destruction of red blood cells as the parasites multiply inside of them. After several days of illness, hemoglobinuria arises and blood appears in the urine. Atypical clinical symptoms can be nervous, respiratory, digestive, cutaneous, or visual. The course of the disease is short: one week at the most. The dog becomes worse if untreated and falls into a coma leading to death. There is a chronic form of the disease, found mainly in adults, that can follow an acute form. The fever is not as high, or is absent, and the overall condition of the dog remains good.
Anaemia is always clearly present. This is a slow form of babesiosis, and complications may occur. The disease may last several weeks and end with the dog's death.
Diagnosis is made based on the presence of fever and anaemia. The dog's lifestyle should be taken into account. Microscopic examination of the blood can confirm the diagnosis. A blood sample is taken from a peripheral area-usually the ear-and examined for the presence of Babesia in the red blood cells. The parasites are more difficult to find in the chronic forms of the disease, since there are fewer in the blood.
There are treatments specific for Babesia, of which the most frequently-used is imidocarb. Sometimes two injections at an interval of forty-eight hours are necessary, since there is a risk of relapse. In addition to this specific treatment, the symptoms of the disease can be treated, particularly the
anaemia (by means of antianemic agents, or blood transfusions in the most serious cases).
Prevention is still the best cure. The disease can be prevented by destroying all ticks as early as possible, and by using acaricide (anti-tick) treatments.
There is a vaccine for babesiosis, but it is effective for a maximum of only six months.
Furthermore, the vaccine is only about seventy percent effective, and can make diagnosis more difficult, for example, if the animal suffers from chronic babesiosis. Two injections are required, three weeks apart. The dog must be in good health and fast for twelve hours before receiving the vaccine. |